Cognitive-behavioral therapy helps clients learn emotional coping in addiction recovery.
Individuals in recovery will have a lifelong journey toward healing. But, they must equip themselves with life skills to maintain sobriety after rehabilitation.
CBT changes old ways of thinking to create healthier behaviors in a sober life.
This article will cover key questions you may have about CBT:
- What is cognitive behavioral therapy?
- What is the difference between CBT and DBT?
- What are the types of CBT?
- What techniques are used in CBT?
- What should I know before starting CBT?
As always, we like to start you off with the basics.
What is Cognitive Behavioral Therapy (CBT)?
Cognitive Behavioral Therapy defines a group of similar talk therapies designed to reform emotions. CBT guides coping methods and emotional regulation for facing life challenges. Session structure allows clients to reveal problems, set goals, and practice healthy skills.
CBT is a method used in many counselor-guided mental health treatments. Clients attend sessions to discuss and address any emotional pain or troubling behaviors.
For this conversation, we’ll focus on CBT treatment for addictions.
Individuals with addictions usually engage in CBT in their journey to lifelong sobriety.
CBT can help individuals in recovery if they:
- Currently struggle to control their behaviors around addiction triggers.
- Have difficulties with committing to or finishing day-to-day tasks.
- Have low self-esteem, anxiety, and/or depression.
- Are dealing with social issues due to their emotions, thoughts, or behaviors.
CBT can be a great primary intervention point in addiction. Some clients with severe conditions may need medical treatment or protection first.
What is the Difference Between CBT and DBT?
CBT and DBT are common psychotherapies in addictions treatment. Distinguishing the two can make treatment easier to understand.
Cognitive-behavioral therapy (CBT) focuses on a client’s internal response to challenges. CBT guides clients to choose healthier responses to challenges beyond their control. Clients learn how to use their thoughts, feelings, and behaviors as tools.
Dialectical behavioral therapy (DBT) is a CBT derivative for understanding coping with external triggers. Clients explore emotionally-extreme responses in their relationships. These clients learn to attach healthier coping to these situations.
Treatments may blend therapy methods to cover a client’s challenges.
DBT methods might be right for treatment if the client…
- Demonstrates impulsive or self-harm behaviors.
- Endure intense emotions with romantic partners, family, and/or friends.
CBT serves as a foundation for most therapeutic addictions treatments. Regardless of therapy type, CBT methods will be at the core of most psychotherapy plans.
CBT Explained
Many therapies fall under the umbrella of CBT. This term is a sort of “swiss army knife”, with its branches offering specialized care to meet client needs.
Cognitive behavioral therapy as a category unites under a few core similarities.
Format of CBT is a type of psychotherapy, or talk therapy. Psychotherapy allows clients to discuss their emotions, thoughts, and difficulties with a counselor.
Structure is significant in making goal-based improvements in the client’s life. The client uses CBT to help them overcome their maladaptive thoughts.
Length of treatment varies but is usually short-term with an average of 16 sessions. Limited treatments better equip clients to handle challenges independently.
Common format variants on the classic one-on-one individual therapy include:
- Group CBT involves a collective treatment of peers with similar challenges.
- Family CBT integrates the client’s family into therapy to address issues in the home unit.
Since CBT is a therapy category, we’ll need to explore the types of therapy it includes.
Types of CBT
CBT is inclusive of many specialized therapies to meet unique struggles in clients.
Above all else, the basics of CBT combine the approaches of:
- Cognitive therapy broadly confronts a client’s emotion-thought relationships to foster healthier coping.
- Behavior therapy hones in on a client’s learned behaviors and environmental conditioning.
Many therapies within the CBT umbrella were created to expand on this foundation.
In the scope of CBT-based therapies, there are a few notable types.
Dialectical Behavior Therapy (DBT) builds new coping methods for emotionally-extreme relationships.
Rational Emotive Behavior Therapy (REBT) helps clients modify their irrational beliefs. Clients identify, challenge, and learn from their maladaptive beliefs.
Multimodal Therapy addresses each of one’s unique personality aspects. These “modalities” include biology, relationships, thoughts, feelings, behaviors, and more.
Cognitive Emotional Behavioral Therapy (CEBT) extends basic CBT focused on emotionally unhealthy coping.
Moral Reconation Therapy (MRT) boosts moral logic to lower criminal reoffending.
Crossover between types of therapy is not uncommon. When a client receives therapy labeled as “CBT,” they may engage in techniques across types.
Skills Learned in CBT
Clients involved in CBT are intended to learn skills for mental awareness and coping.
CBT life skills may take forms including, but not limited to:
Conceptualization helps clients identify and discuss the problems a client is experiencing. This is a client-therapist collaboration that helps with setting goals.
Automatic thoughts awareness identifies maladaptive beliefs in response to triggers. Automatic negative thoughts are specifically targeted and analyzed.
Acceptance teaches clients to embrace their past as is and improve the present. Clients release things outside their control to improve their self-talk “here and now.”
Functional Analysis dissects the roots and results of the client’s behaviors. A client learns to identify triggers of dysfunctional behaviors and shape their reactions.
Ultimately, clients learn how to change their behaviors and solve their life challenges.
This skill-building begins with a client attending therapy sessions.
CBT Sessions Explained
Process of CBT sessions is structured to teach a client how to solve their own issues.
A client will attend sessions and talk with a therapist about their challenges. The therapist helps the client to identify problems and set goals for solutions.
The process can be simplified into a few main steps:
- Identify problem areas in life.
- Develop awareness of thoughts/emotions/beliefs in these areas.
- Identify negative or inaccurate thinking.
- Reshape negative thoughts/faulty thoughts.
Techniques used to explore a client’s challenges can include:
Feedback evaluates symptoms and notes how often a client displays desired behaviors. The therapist guides the client based on these areas.
Role-playing engages the client in mock interactions with a therapist. The therapist acts as a figure in the client’s life to understand the nuances of the client’s challenges.
Mindfulness helps the client focus on aspects of being “present” to improve acceptance. This awareness of body and mind state improves reactions to issues.
Exposure therapy trains healthier coping by gradually increasing a client’s exposure to triggers. Every step analyzes a client’s responses and sets goals for better reactions.
Challenging beliefs can help clients understand alternatives to their automatic thoughts. By learning to pause before reacting, a client can choose better thoughts.
This process cannot be completed in therapy alone. A client is tasked with post-session “homework” to explore their obstacles independently. After all, fighting addiction is a full-time job.
CBT “Homework” Explained
CBT homework includes life skills and self-reflection practice without a therapist’s guidance.
This may also be called an “action plan.”
The process of CBT homework is:
- Completing practical tasks to reflect on or practice in-session takeaways.
- Return to therapy with new insights and new themes to work on.
- Complete new homework based on the discussions in therapy.
A few examples of home a CBT may assign:
- Cognitive-behavioral journaling to log thoughts, emotions, and behaviors. This allows a client to examine themselves and identify areas to work on.
- Skills practice allows the client to apply new coping methods in real-life situations. The results are noted and discussed in therapy.
The cycle of sessions and homework is key to getting real, long-term results in CBT.
Other Disorders Treated by CBT
Clients may enter CBT for addictions recovery.
But, they often find help coping with other challenges in their life as well.
Some disorders and challenges treated by CBT can include:
- Anxiety
- Depression
- Panic attacks
- Anger management
- Post-traumatic stress disorder (PTSD)
- Sleep disorders
- Sexual issues
- Dual diagnosis
CBT builds resistance against replacing one unhealthy way of coping for another.
Where CBT Falls in the Continuum of Addiction Care
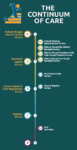
The continuum of addiction care provides intervention at every stage of recovery. An individual follows treatments and referrals to stay on-track towards full independence.
The stages in the continuum of addiction care are:
- Level 0.5: early intervention services
- Level 1: outpatient services
- Level 2: intensive outpatient or partial hospitalization services
- Level 3: residential or inpatient treatment services
- Level 4: medically managed intensive inpatient treatment services
CBT is often present across multiple phase of the continuum depending on the client’s needs.
Individuals usually enter therapy after detox.
Once recovery begins, individuals may start CBT standalone or as part of a program. CBT can be a primary intervention “compass” for gauging next steps.
During recovery, one may return to CBT if experiencing challenges or a relapse.
What to Know Before Starting CBT
Considerations should be taken regardless of where the client starts CBT treatment.
Confidentiality is provided only if the client is not a danger to themselves or others. This includes risk of self-harm, harm to others, or inability to safely care for themselves.
Therapist-client partnership is important for listening, connecting, and confiding. Just note it may not be a main focal point unless the client is in DBT.
Improvement requires committed practice. Change is a lifelong journey when maintaining sobriety, and perfection is impossible. So, be prepared to make mistakes.
When one has decided to begin CBT, there are a few tasks they’ll need to handle.
How to Choose A CBT Program
CBT-inclusive recovery programs may vary in intensity and accessibility.
In-person therapy is the classic format for CBT sessions. Clients meet with a therapist at a physical location, which may vary based on program type.
Inpatient programs may include CBT alongside medical services.
Outpatient programs like IOP may include CBT therapies for rehabilitation.
Standalone sessions are best paired with minimal outpatient services, such as sober living.
Online therapy is usually only available in outpatient services or standalone. These sessions may be offered via video chats with a therapist or online exercises.
“Self-Help” provides CBT principles via books, habit change, mindfulness, and more. Therapy is usually the best choice, but these are highly accessible and affordable.
If local accessibility of CBT is limited, an out-of-state program may be an alternative.
Benefits of an Out-of-State CBT-focused Recovery Program
Out-of-State recovery programs with CBT provide benefits beyond treatment access.
Here are some key benefits and opportunities:
- Remote treatment removes clients from toxic triggers in their community.
- In-person treatment for a better connection to the therapist.
- Unique programs combining services, like IOP plus sober living.
Clients with commitments like caring for family may not find OoS programs viable.
An ideal client would be seeking outpatient services away from their environmental obstacles.
Questions to Ask Before Choosing a CBT Therapist
Finally, clients should ask questions with their potential therapists before selecting.
There may be a few important points to consider:
Is the therapist certified? A CBT therapist should be a licensed mental health professional. While not required, further training beyond licensing also exists. NACBT provides some of the popular certifications like:
- Diplomate in CBT
- Certified Cognitive-Behavioral Therapist
- Certified Cognitive-Behavioral Group Therapist
- Certified Cognitive-Behavioral Group Facilitator
Do I feel comfortable with the therapist? Clients should find a therapist that fits. A bit of apprehension is normal, but one should trust their gut. If they’re not able to open up to this person, recovery will be stunted.
Am I ready to be uncomfortable and honest with myself? Therapy only helps if the client surrenders to it. One may want to take note of their challenges to prepare. Logging difficult thoughts and emotions can be a good starting point for therapy.
Can this therapist address my specific issues? Clients should match specific issues with the therapist’s specialties. Does their background match the client’s needs? One may want to ask about the types of clients the therapist normally works with.
Takeaways on Cognitive Behavioral Therapy
In summary, CBT for addiction is a strong method for lasting rehabilitation.
By now, you’ll have learned that:
- Cognitive-behavioral therapy is an umbrella term for many different therapies.
- DBT extends CBT methods to focus on relationships and emotional validation.
- CBT comes in many types, and may even blend due to similar principles.
- Clients learn emotional coping via techniques like roleplay and mindfulness.
- Anyone seeking CBT should take time to find the program for their needs.
Ultimately, CBT can be a major step in one’s journey with Next Step Recovery, to persisting in sobriety.
Know someone who could benefit from learning about cognitive behavioral therapy? Please like and share this post with them. Or, leave your questions or comments about the CBT below! We’re always looking for ways to keep the conversation about recovery going. Education is one of the most powerful tools we have to fight addiction.









