Dialectical behavior therapy helps those in recovery find a healthier state of mind.
Individuals on the journey to recovery will find themselves healing for a lifetime. Therapy equips them with skills to stay sober and independent after early recovery.
DBT focuses on aspects of acceptance and change in sobriety.
What this article will cover:
- What is Dialectical Behavior Therapy?
- How are DBT and CBT different?
- How do DBT skills help in addiction recovery?
- How do DBT treatment sessions work?
- How does DBT relate to the continuum of addiction care?
- What should I know before starting DBT?
Before we dive deep, we always like to start you off with the basics.
What is Dialectical Behavior Therapy (DBT)?
Dialectical Behavior Therapy (DBT) integrates cognitive-behavioral therapy with Buddhist-based mindfulness. It is a talk therapy designed by 1980s psychologist Marsha M. Linehan. DBT validates emotional sensitivity that can block the transformation of maladaptive thoughts and behaviors.
DBT is a common therapy method in many modern mental health programs. It is used to manage extreme emotions and make behavioral changes for a healthier life.
In this discussion, we’ll talk about DBT for addiction treatment.
Individuals in addiction recovery might be in DBT as they move towards sobriety.
DBT can help individuals in recovery if they:
- Feel out of control with their behavior around addiction triggers.
- Find that daily tasks are difficult to start or complete.
- Have any thoughts of or attempts at self-harm or suicide.
- Have impulsive reactions in emotional stress, especially social relationships.
- Do not have an intellectual disability or unregulated schizophrenia.
DBT is a powerful early intervention treatment for addiction care. Clients will likely be placed in protective care before proceeding if at-risk of harm to themselves or others.
What is the Difference Between DBT and CBT?
DBT and CBT are similar psychotherapies, but differ in how they approach emotions.
Dialectical Behavior Therapy (DBT) is an expansion of CBT. It uses the principles of mindfulness “acceptance” and cognitive-behavioral “change” in tandem. Focusing on validating heightened emotions supports lower resistance to changing behaviors.
Cognitive Behavioral Therapy (CBT) is the foundation of therapy in DBT. The goal is to uproot unhealthy beliefs and thoughts for behavior change. But clients may resist if they feel their emotions are being undermined. This is why DBT was developed.
Cognitive behavioral therapy is the basis for many popular psychotherapies. CBT may meet the needs of many individuals. Modified CBT methods like DBT confront specialized challenges.
Clients might be specifically recommended DBT if:
- Extreme emotional sensitivity is present
- They enact impulsive actions with abnormal highs and lows.
- Demonstrates intense emotions with friends, family, and/or in romances.
- They have felt burnout or have been unmotivated during other therapies.
DBT is common in substance abuse recovery treatments. Clients who struggle with extreme emotions may benefit from the mindfulness component of DBT.
DBT Explained
Dialectical behavior therapy is a combination of two mental health methods:
- Cognitive Behavioral Therapy (CBT)
- Mindfulness meditation
DBT addiction programs may operate differently, but most share a few key features.
Format is talk therapy, aka psychotherapy. Clients discuss with a professional counselor their challenges, and how they think, feel, or act due to these stresses.
Structure is based on the client’s self-defined goals. The client confronts their obstacles via skill-targeted sessions called modules.
Length of a DBT program commits clients for six months to a year. Clients complete the main modules once every six months. Clients use DBT post-therapy to stay sober.
As with all behavioral therapies, DBT is defined primarily by the life skills it teaches to clients.
Skills Learned in DBT
DBT skills are meant to blend—or “synthesize”—two seemingly-opposite mental health methods.
This balance and integration of mindfulness acceptance and cognitive-behavioral change is considered “dialectical.”
The core skills are defined within four types of sessions, each referred to as modules.
The DBT skill modules include:
- Core mindfulness is an acceptance-focused skill for keeping the mind in the present moment. Being aware of one’s self and of others helps clients embrace thoughts, feelings, and behaviors without judgment.
- Distress tolerance is an acceptance-focused skill for enduring and accepting pain as is. This helps clients avoid unhealthy emotional reflexes such as substance abuse and self-harm.
- Interpersonal effectiveness is a change-focused skill for supporting healthy assertiveness. Clients learn to respect others as they improve their own self-respect and establish personal boundaries.
- Emotional regulation is a change-focused skill for revealing, understanding, and altering emotions. Clients will learn how to turn destructive emotions into productive ones.
Ultimately, clients progress through modules with the goal of behavior change.
While skill-building is the goal in DBT, the session structure defines how it operates.
DBT Session Structure
DBT sessions are designed to guide clients to their own solutions for their challenges.
Clients receive treatment through various interactions with their therapists and peers.
The four-stage hierarchy of rehabilitation breaks down into:
- Life-threatening behaviors. Clients regain control to halt and prevent self-harm, substance abuse, and other volatile actions.
- Therapy-interfering behaviors. Clients build DBT skills from their new stability to move past emotional inhibitions against recovery.
- Quality of Life. Clients apply DBT skills to relationships, meeting the basic needs of independent living, and other issues.
- Meaningful Life. Some clients will seek deeper fulfillment and life purpose. The client looks for more satisfaction in themselves and from relationships.
Comprehensive DBT breaks this process into three client-facing session types:
- Group therapy educates clients and fosters behavioral practice in a classroom setting.
- Individual therapy allows clients to sharpen their DBT skills against their life issues.
- Phone-in coaching offers 24/7 support for brief, in-the-moment emotional challenges.
A fully comprehensive DBT program also has the therapists and other provider staff engage in their own care program via:
- Consultation team sessions help providers with motivation and problem-solving as they treat clients.
The full experience would have clients engage in all formats. This covers many clients’ social and personal challenges in a safe, controlled environment.
However, DBT is a flexible therapy that can be delivered in different configurations.
Non-comprehensive DBT programs treat clients with a partial set of session types. Some popular programs offer individual-only or group-only. Others may use phone coaching from a crisis hotline instead of the client’s therapist.
Since comprehensive DBT is ideal, it’s best to understand each of its session types.
DBT Group Sessions Explained
Group DBT sessions are peer-based life skills training in a classroom setting.
In these sessions, clients work on behavioral rehabilitation by learning DBT skill sets.
Learning and practicing with others on similar obstacles offers personal insights. As a result, communal growth and collaboration can ease resistance to change.
Techniques used may include:
- In-class behavioral role-play to learn to act healthier on thoughts and feelings.
- Homework “diary cards” to follow emotions and DBT skills used and determine progress.
Duration of these sessions is around two to three hours each week.
Frequency of group therapy is weekly, for an average length of six to 12 months.
DBT Individual Therapy Sessions Explained
Individual DBT sessions are one-on-one for personalized treatment, skill-building, and guidance.
Intimate single-client sessions help clients find their vulnerability to confide and learn. Clients begin to attach the DBT skills to their specific struggles and perceptions.
Techniques applied for these psychotherapy sessions may include:
- In-session client-therapist dialogues with a direct focus on the client’s specific struggles.
- Homework “diary cards” like those used in group therapy to trace their mental experiences and any DBT skills used.
- Homework task assignments to practice working through mental hurdles independently.
Duration for each session is roughly 60 minutes on average.
Frequency of one-on-one therapy sessions is once per week for six to 12 months.
DBT Phone-In Sessions Explained
Phone-in DBT coaching sessions are short phone calls for situational guidance.
With phone coaching sessions, clients get “real-time” help as they navigate a challenge in-the-moment.
Remote one-on-one calls give clients instantly actionable tips to maintain healthy behaviors. Clients need this most when faced with volatile, intense emotions. This might include being tempted towards impulsive behavior.
Duration of a phone session is normally just a few minutes. It is long enough to provide an immediate DBT technique to apply to the client’s current issue.
Access to the client’s therapist is usually 24-7 in true comprehensive DBT. Some programs may offer the number to a crisis line instead. However, clients should note that many crisis line operators are not equipped to run through DBT methods.
Each session format works together to treat addictions and other disorders as well.
Other Disorders Treated by DBT
Alongside substance use, it is common for the client to have dual diagnoses.
Fortunately, DBT may help in treating more than just a client’s addiction.
DBT is ideal for clients that are hard-to-treat due to emotional struggles or even multiple disorders.
This therapy was created in the 1980s to treat Borderline Personality Disorder (BPD).
The scope of dialectical behavioral therapy has since expanded to include:
- Clinical depression (treatment-resistant major depression, chronic depression, etc.)
- Post-Traumatic Stress Disorder (PTSD)
- Eating Disorders (Binge eating, bulimia, etc.)
- Attention-Deficit/Hyperactivity Disorder (ADHD)
- Bipolar disorder
- Generalized anxiety disorder
- Suicidal and self-harming behavior
DBT might be delivered in combination with other treatments to provide full care.
How DBT Relates to the Continuum of Addiction Care
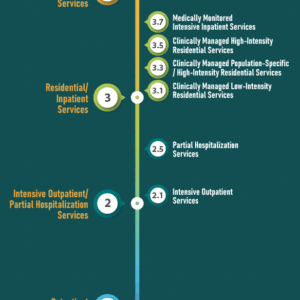
The continuum of addiction care is the framework for seamless treatment. Clients enter a sequence of interlocked programs and referrals to gain full independence.
The main stages in the continuum of addiction care are:
- Level 0.5: early intervention services
- Level 1: outpatient services
- Level 2: intensive outpatient or partial hospitalization services
- Level 3: residential or inpatient treatment services
- Level 4: medically managed intensive inpatient treatment services
DBT can be included in a client’s treatment plan all along the continuum.
Individuals usually must go through detoxification before therapy can begin. It’s also not uncommon to enter residential or medically-managed protective care first.
When in recovery, clients typically use a combination of addiction therapies to regain control and practice healthier living.
Beyond recovery and even into independence, some clients return to therapy. These clients may need to work through unresolved challenges or even a relapse.
What to Know Before Starting DBT
Before starting a DBT program for addictions, clients should know what to expect.
Commitment is required via a signed agreement before a client can even enter many DBT programs. Clients should be ready to give time and attention for six to 12 months of psychotherapy. This includes consistent attendance and homework.
Confidentiality may be reduced if the client is at risk for harm to themselves, others, or unsafe self-caretaking. DBT deals with extreme emotions that may connect to physically harmful behaviors. So, providers may need to disclose some information.
Provider-client relationship is essential to the client’s progress in DBT sessions. Clients should always be ready to listen, learn, and speak openly to get the best care.
If a client decides to commit to DBT, they’ll have some important choices to make.
How to Choose a DBT Program
DBT treatment programs vary, allowing clients to match a program for their needs.
In any case, clients will enter a treatment program based on the severity of their condition and access to services.
In-person sessions come in a few program formats:
- Inpatient programs include DBT alongside hospitalization or clinical-monitored residential care.
- Outpatient programs may pair DBT with an intensive care or residential housing like sober living homes.
- Standalone sessions may be accessed without entering in-depth addiction treatment programs.
Online counseling via remote sessions on video, phone, and/or text. Online clients may have limited in-person options or need scheduling flexibility. Be sure to find programs with online group sessions along with traditional individual therapy.
“Self-help” services like books and other media may be best as a supplement to an actual treatment program. The therapist-client relationship and group sessions being important to progress. Self-help excludes these essential social supports.
Regardless of program, some clients may temporarily relocate for better care.
Benefits of an Out-of-State DBT-focused Recovery Program
DBT-inclusive recovery away from home may offer better treatment access.
Some of these advantages include:
- Removal from addiction triggers in the client’s home environment.
- Face-to-face treatment for a better emotional connection to providers.
- Fully integrated “continuum of care” services—like IOP with sober living.
- Emotionally resetting in a new community to give clients a new perspective.
Clients who cannot relocate for months may not be ideal for OoS recovery programs. This might include any primary caretakers of children or disabled loved ones.
However, many OoS clients value having distance from their triggers.
Questions to Ask Before Choosing a DBT Therapist
With any program, clients should talk with their therapist to see if they will get the care they need.
Potential DBT clients might ask their therapist the following:
Do you specialize in DBT? DBT therapists should have experience and training from a reputable DBT education program. Firsthand training is ideal, like those from Behavioral Tech via the DBT developers themselves.
Are you certified in DBT? While not required, clients may feel more comfortable if their therapist has the certification. Look for credentials from the Linehan Board of Certification (DBT-LBC).
Is this “true” comprehensive DBT? Comprehensive DBT involves an all-inclusive combo of services. This means 24/7 phone coaching, weekly individual therapy, and weekly group sessions. Some programs exclude services or vary their frequency.
Does this DBT program provide support to the care providers? Comprehensive DBT gives the therapists their own consultations and support for their challenges. These may include care-providing hurdles or their personal mental struggles.
Is my phone coach DBT-trained? The client’s coach may not be their primary therapist. However, they should still be receiving real DBT coaching when they call. Some facilities cannot afford the time or costs for DBT training and 24/7 availability.
Am I ready to commit to 6-12 months of hardcore self-reflection? Commonly, clients will agree to a signed commitment of six to 12 months for DBT sessions. These programs may require relocation, so not all clients can commit.
Am I comfortable with this person? Clients should feel at ease opening up to their therapist.
Takeaways on Dialectical Behavior Therapy
In summary, DBT can equip addiction clients with skills for a lifetime of sobriety.
From this article, you should now know that:
- Dialectical behavioral therapy blends CBT methods and mindful awareness.
- DBT confronts emotional resistance that disrupts other CBT-based therapies.
- Skills learned in DBT help clients take back their life from maladaptive coping and impulsive behaviors.
- DBT sessions come in a four-part system. This includes group therapy, individual therapy, phone coaching, and consultation team support sessions.
- DBT can act as a behavior intervention at any point after detox— including after full independence.
- Clients should always at least check that their therapy program is comprehensive. Also, check that the therapist is professionally DBT-trained.
Ultimately, DBT can be the foundation clients at Next Step Recovery who need to progress into recovery.
Know someone who could benefit from learning about dialectical behavioral therapy? Please like and share this post with them. Or, leave your questions or comments about the DBT below! We’re always looking for ways to keep the conversation about recovery going. Education is one of the most powerful tools we have to fight addiction.









